As I navigate this journey I realize that there are so many people out there who are trying to navigate the same waters. So, I wanted to take a step back and share how I was diagnosed with thoracic/diaphragmatic endometriosis in case there are others who need this right now. I had an ablation in…
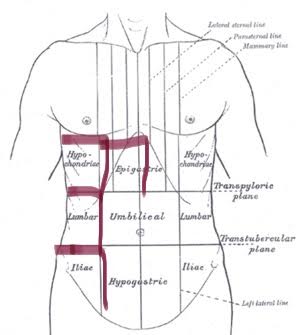
How They Diagnosed Me With Diaphragmatic Endometriosis