We have this notion - or perhaps a false hope - that excision surgery is going to miraculously take away all the pain and suffering leading up to this day. And, while excision is the gold standard of diagnosing and treating endometriosis, it is always good to be prepared for lingering AND new symptoms that…
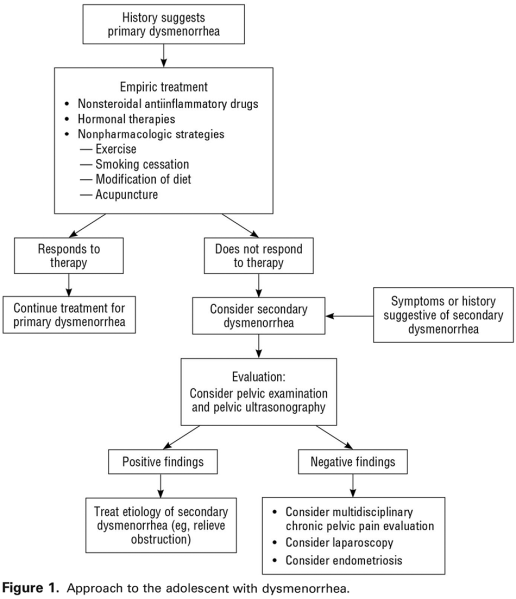
Primary vs Secondary Dysmenorrhea